Prolapse And Pelvic Floor Repair
PROLAPSE AND PELVIC FLOOR REPAIR
Consult the Best Gynecological Laparoscopic Surgeon in Lahore.
With years of experience in Gynecology, we are here to help
Our Specialist Gynecological Laparoscopic surgeons are specialized in all kinds of:
Laparoscopic Prolapse And Pelvic Floor Repair
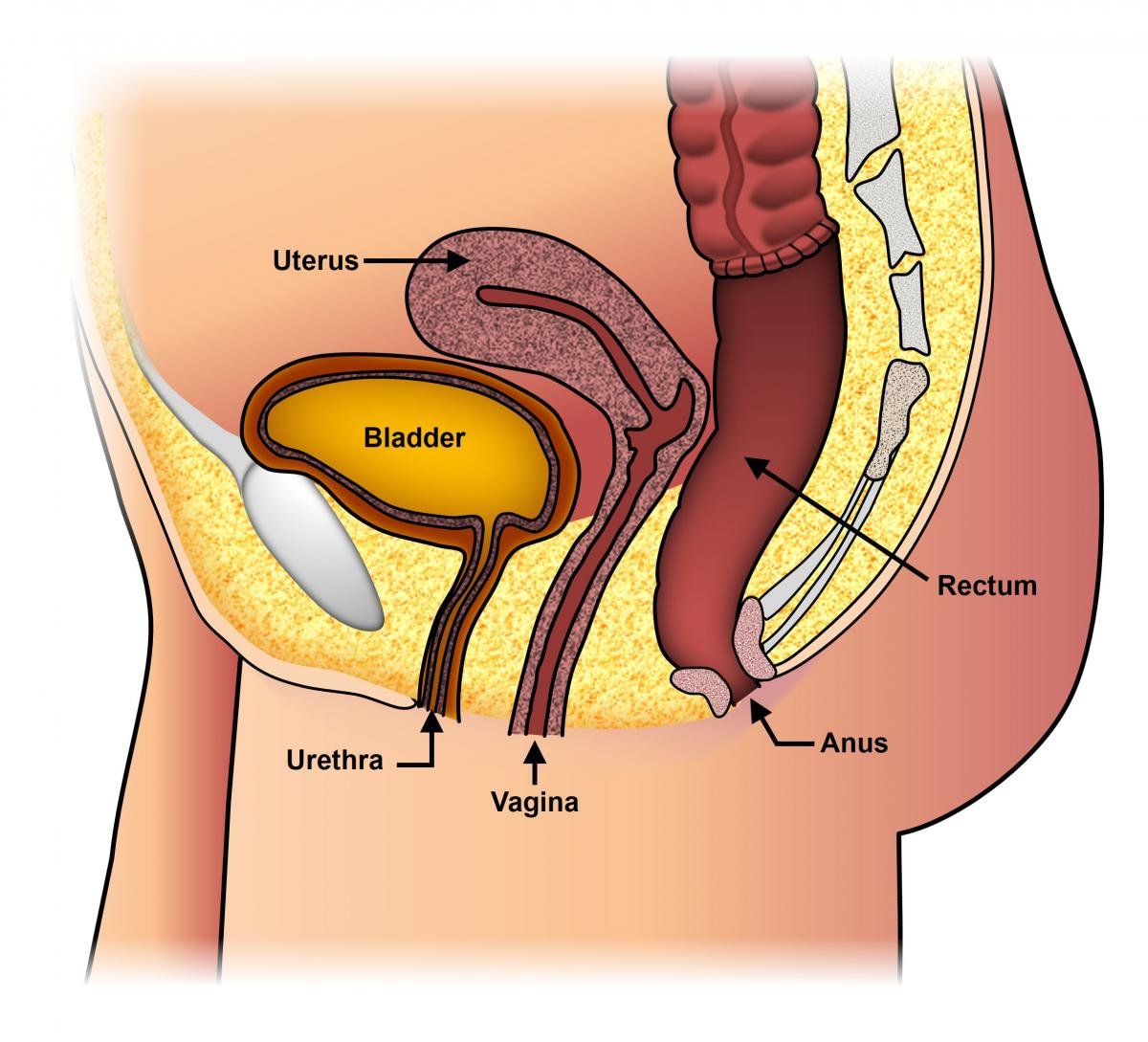
Laparoscopic pelvic organ prolapse surgery is a minimally invasive procedure used to treat pelvic organ prolapse, which is a pelvic organ that sags down and compresses the vagina, causing a bulge or mass.
Pelvic organ prolapse surgery is used to restore the normal structure and function of these pelvic organs and relieve symptoms including pain, discomfort, pressure, and urinary and bowel dysfunction.
Laparoscopic pelvic organ prolapse surgery uses very small specialized surgical tools inserted through small incisions in the abdomen, allowing surgeons to view and manipulate pelvic organs without using long incisions.
PROLAPSE AND PELVIC FLOOR REPAIR
Why do you need this Laparoscopic Prolapse And Pelvic Floor Repair?
The main purpose of surgery is to relieve symptoms of vaginal flatulence/relaxation and improve bowel function without affecting sexual function. however, there is a chance that another part of the vaginal wall prolapses or prolapses can recur. Special measures are taken in the form of fixation of specific tissues during laparoscopic procedure to avoid recurrence
Consult the Best Gynecologist in Lahore for your Laparoscopic Prolapse And Pelvic Floor Repair
Consider surgery if the prolapse is causing pain, if you have bladder and bowel problems, or if the prolapse makes it difficult for you to perform activities you enjoy. Organs may sag again after surgery. Surgery in one part of the pelvis can worsen the prolapse in another.
This minimally invasive approach has several advantages over vaginal methods or traditional open surgery, including:
PROLAPSE AND PELVIC FLOOR REPAIR
Types of Pelvic Organ Prolapse
Depending on the type of prolapse, there are several procedures to correct pelvic organ prolapse:
Pelvic Prolapse Repair
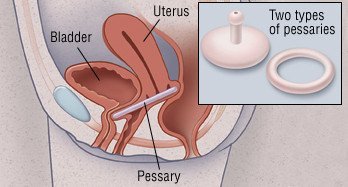
For many women, prolapse can involve a descent of the uterus, vagina, bladder, and/or rectum, resulting in a "bulky" feeling in the vagina. In some cases, these organs may stand out significantly. Pelvic organ prolapse can lead to symptoms such as leaking urine, constipation, and dyspareunia.
Laparoscopic vaginal suspension is a minimally invasive surgical technique that provides a safe and permanent way to reconstruct the pelvic floor and its contents without the need for large abdominal incisions.
Procedure Of Laparoscopic Prolapse and Pelvic Floor Repair
Laparoscopic vaginal suspension is performed using endoscopic micro instruments inserted through 4 keyhole incisions in the mid-abdomen.
In the case of pelvic organ prolapse, the vaginal supports loosen, causing the pelvic organs to protrude. The purpose of laparoscopic vaginal suspension is to resuspend the vagina and associated pelvic organs through a keyhole incision. In some cases, simultaneous hysterectomy, bladder suspension, or rectocele repair may be required. All of which can be completed via a vaginal course.
Laparoscopic Vaginal Suspension is a well-established procedure at our hospital and is performed with the help of an experienced and dedicated laparoscopic surgical team, including nurses, anesthesiologists, operating room technicians, and many of them will be met on the day of surgery.
How is it done?
A vaginal suspension is made laparoscopically through 4 small incisions (0.5-1 cm) in the middle of the abdominal cavity. Through these small incisions, tiny endoscopic instruments for dissection and suturing are inserted. Excellent visualization of the pelvic organs is achieved using a high-power telescope lens attached to the camera device, which is inserted into one of the keyhole cutouts.
The vaginal and pelvic organs are then resuspended inside with sutures and support mesh or fascial grafts. If necessary, bladder suspension, vaginal hysterectomy, and rectocele repair can be performed simultaneously through a vaginal incision. A Foley catheter (i.e. a bladder catheter) is placed to drain the bladder.
Urinary incontinence: Incontinence that was already present at the time of surgery is usually treated with bladder suspension, but minor incontinence may remain and usually resolve over time. Sometimes, medication may be required.
The length of the procedure for laparoscopic vaginal suspension varies from patient to patient (3-5 hours), depending on internal anatomy, pelvic shape, patient weight, and because of previous abdominal/pelvic infection or the presence of scarring or pelvic inflammation. Operation.
The blood loss of laparoscopic vaginal suspension is usually less than 200 mL, and blood transfusions are rarely required.
PROLAPSE AND PELVIC FLOOR REPAIR
Possible Risks and Complications
Although the laparoscopic vaginal suspension is very safe, as with any surgical procedure, there are potential risks and complications. Possible risks include:
Bleeding:
Although blood loss during this procedure is relatively low compared to open surgery, blood transfusions may still be required if deemed necessary during surgery or the postoperative period.
Infections:
All patients were treated with intravenous antibiotics before the start of surgery to reduce the chance of infection in the urinary tract or at the incision site.
Adjacent tissue/organ damage:
Although uncommon, possible damage to surrounding tissues and organs, including the gut, vascular structures, pelvic muscles, and nerves, may require additional surgery. During surgery, transient damage to nerves or muscles may occur concerning the patient's position.
Hernias:
Hernias rarely occur at the incision site because all keyhole incisions are closed under direct endoscopy.
Urinary retention:
Like incontinence, postoperative urinary retention is uncommon and usually occurs in patients who also undergo bladder suspension. Intermittent self-catheterization may be required after surgery.
Things you should know before Laparoscopic pelvic floor repair
Laparoscopic pelvic floor repair refers to the use of laparoscopy or minimally invasive surgery to correct pelvic organ prolapse.
Over the past decade, physicians have used laparoscopic surgery to diagnose and treat most gynecological conditions. In the process, doctors have discovered that laparoscopy can help identify and repair the many different defects that cause pelvic organ prolapse and return them to their normal positions.
In traditional revision surgery, an incision is made through the vaginal skin, and the torn or damaged connective tissue is covered with absorbable sutures.
In laparoscopic pelvic floor repair, the surgeon reconnects the prolapsed pelvic organ to the pelvic floor muscle or bone landmarks using a nonabsorbable/permanent mesh material or thread.
This repair is based on the concept that pelvic organ sagging is primarily due to shear forces destroying the connective tissue that connects the pelvic organs to the pelvic floor.
Laparoscopic surgery is indicated for the correction of the types of pelvic floor dissection defects that constitute bladder prolapse, hydrocele, uterine prolapse, and post-hysterectomy fornix prolapse.
The benefits of laparoscopic pelvic floor repair include a high success rate (over 90%), less postoperative pain, and a reduced risk of vaginal scarring and vaginal strictures.
Common risks with laparoscopic pelvic floor repair are unusual. They include risks associated with anesthesia, laparoscopic surgery, and vaginal repair. The latter may involve rare damage to the bladder, bowel, blood vessels, and pelvic nerves.
Because every patient has different types of pelvic floor defects, different tissue qualities, different health conditions, and different outlooks, you should consult with your specialist to determine if laparoscopic pelvic floor surgery is right for you.
PROLAPSE AND PELVIC FLOOR REPAIR
Consult the the expert Laparoscopic surgeon in Lahore today and get your treatment in the best way possible.
At us, you will have expert surgeons who have special skills in laparoscopic pelvic floor repair have taught and demonstrated these techniques at numerous national and international platforms. So, consult us today for a better future.